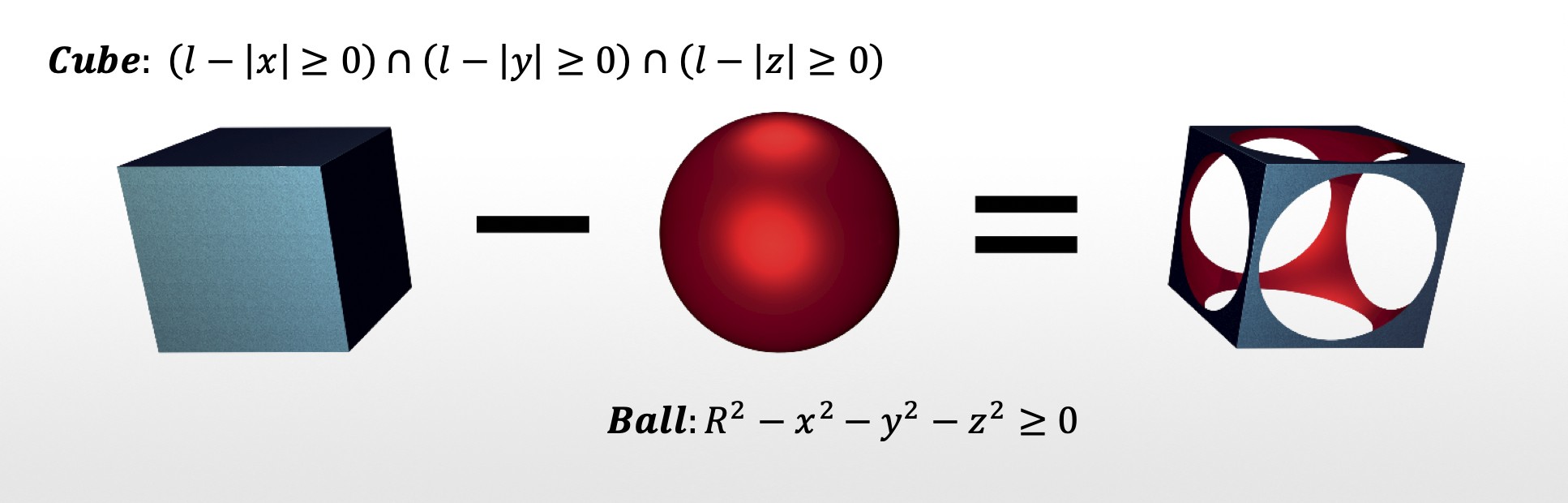A novel efficient method of biomedical implants design and manufacturing was developed at the Skoltech Center for Design, Manufacturing and Materials (CDMM), in the scope of a multidisciplinary research. The research results were published in Applied Sciences journal.
Complex-shaped biomedical implants for replacing bone defects are often manufactured from ceramic materials to provide the necessary strength to the injured bone region, reduce inflammation, and facilitate living cells proliferation and osteogenesis. The living cells are expected to reach the internal space of the implants, attach to the surface and enable the tissue regeneration process. To give access to internal regions, the implants must be porous, with pore size of tens to hundreds of microns. The pores must span through the entire volume of the implant. The size and geometry of the pores is hard to regulate in traditional manufacturing approaches. Additive manufacturing technologies allow on-demand variation of every single pore for precise fit to the microstructure of the surrounding bone tissue and optimization of cells regeneration.
It took an advanced expertise of three CDMM research groups, working in different fields, to accomplish this endeavor. The overall concept and design of the implants were developed by the Ceramics Additive Manufacturing (AM) team of Dr. Svyatoslav Chugunov and Andrey Tikhonov, based on specifications from a partner medical institution. The preliminary development of CAD models of the implants revealed the shortcoming of the conventional modeling approach. The CAD-based parameterization was giving up on variation of the pores, strut thickness and morphology of basic element intersections in the designed models. While it is possible to develop a few static models of an implant, the CAD model allows no easy changes in the grid-like implant topology, when tailoring of the structure to a particular customer is required.
To provide the flexibility to the geometry and gain a parameterized control over every element of the porous structure, the team of Prof. Alexander Pasko, Dr. Evgenii Maltsev, and M.S. Dmitry Popov was involved to help modelling the implants with the Function Representation (FRep) modelling approach. This method is based on geometry representation with mathematical functions. For example, can you imagine a mathematical description of your teapot or a сup? FRep allows you to represent it mathematically. The basic building blocks, such as spheres, cubes, cylinders, and others, are represented with equations. The morphological and topological operations (rotation, translation, merging, cutting, intersecting, etc.), applied to the basic elements, are expressed via mathematical operations over the equations that represent these elements. Combining all the equations and operations in a special order, a sequence of mathematical formulas could be derived that represents geometrical objects of very complex shape (Figure 1). In a numerical script this sequence is expressed with just a few lines of a code. Additional operations such as cycles, region copying and translation operations, help to automate generation of periodic structures for huge volumes, while the length of the script remains quite short. FRep combines many different geometric modeling techniques, ranging from implicit surfaces and Constructive Solid Geometry to procedural 3D modeling.
At every level of FRep modeling parameters could be introduced into the equations and mathematical operators. These parameters help to adjust any part of the modeled geometry at any stage of the modeling. The equations, representing the basic elements could refer to not only the geometry, but also to materials. Applying mathematical operations to equations, representing materials, heterogeneous objects could be created, including the ones with density gradient. Of course, this process can be efficiently parametrized too. The use of parameters allows introduction of changes to periodic structures on the fly or modification of any of the selected element within the periodic structure to introduce individual features (Figure 2).
The geometrical object from FRep-based form can be exported to a variety of different file formats, including the STL. The STL files could be used with any slicing software to prepare the model for 3D-printing.
The biggest advantages of the FRep method over a conventional CAD modeling are in advanced parameterization of every modeled entity, the easy representation of complex geometries in the form of a few lines of a numerical code, and the possibility to create computer or mobile apps that allow generating complex geometrical items, adjusting the topology and morphology of the geometry with a simple tweak of sliders in a GUI, and exporting the result to an STL-file, ready for 3D-printing (Figure 3). The compilation of such an application with FRep is a fast and straightforward task that is often accomplished in 1-2 days for 4-5 parametric models. When the GUI-featured app is prepared, the operations on design of implants and tailoring their structure to particular use-cases could be done by even a user unexperienced in CAD or 3D-printing. The exported STL file requires only minimal adjustments, specific to a particular 3D-printer, to get ready for production.
The bone-replacing implants have to be strong enough to sustain the mechanical stresses, experienced by the bone or the load exerted by external objects upon a contact. Thus, mechanical strength of the implants is of great importance. The numerical study of mechanical behavior and material failure scenarios of the implants was performed by the team led by Prof. Alexander Safonov of Composite Materials lab at CDMM, using ABAQUS finite element modeling suite. According to medical partners, the primary load scenario for these types of implants is the compressive loading. The FRep-generated STL models of implants were evaluated with ABAQUS for compressive strength and the possible failure regions were predicted. The difference between numerical and experimental results did not exceed 5%.
Armed with the numerical results, the Ceramics AM team produced four implants of different designs and tested them in Mechanical Testing lab of CDMM, with the help of Stepan Konev (chief engineer). The use of a Digital Image Correlation (DIC) system during the testing enabled an access to the temporal behavior of implants under loading. The use of spatially resolved strain field, computed with DIC, helped analyzing the input of every component of the grid-like structure to the mechanical performance of the specimen, including the moment of material failure. The experimentally determined failure scenarios well matched the numerically forecasted modes. All tested implants fulfilled the requirements; hence the full-blown series of implants were 3D-printed for medical evaluation.
Based on the research results, the FRep method proved to be a great tool not only in generating complex geometrical structures, but also in preparing a visually appealing GUI-based apps that allow rapid creation of many implant models with variation of parameters of every entity of interest. The combination of FRep modeling approach, the FEM-based numerical evaluation procedure, and additive manufacturing technologies lead to development of customized biomedical implants in very short time (typically, 10 days from design to the ready item) and at relatively low cost. The extra advantages provided with the additive manufacturing approach are in manufacturing of complex shaped items and, more important, in manufacturing of tens or hundreds of different customized implants on the same printing platform within one production cycle, which helps addressing great number of different requests within a very short period of time.
The engineering approach demonstrated in this work would be evolved into a well-validated practical instrument for a rapid production of biomedical implants that meet medical requirements and could be efficiently adjusted for every customer. We plan to expand the line of the available ceramic materials. Additionally, a novel method of ceramic 3D-printing for porous structures will be developed to help reducing greenbody post-processing time and improve the quality of the internal regions of the printed parts.
Contact information:
Skoltech Communications
+7 (495) 280 14 81